More Sunlight May Be the Cure to Your Ailments

The sun emits electromagnetic radiation, which encompasses a large spectrum of wavelengths. Of these, only infrared, visible light, and ultraviolet (UV) radiation are able to reach the earth’s surface and hence our skin. So far, most of the research regarding the effects of the sun on human health has focused on UV radiation,1, 2 which is divided into UVC, UVB and UVA.3
As depicted in figure 1, virtually no UVC radiation reaches the earth’s surface, except at extremely high altitudes, since it is efficiently absorbed by the stratospheric ozone layer.1-3 Ozone also absorbs most of the UVB and UVA radiation.
Indeed, only about 0.1% of UVB radiation and 5% of UVA radiation reach the surface of our planet. In contrast, 39% of visible radiation and 56% of infrared radiation can reach the earth’s surface.2 Nevertheless, even these small levels of UVA and UVB radiation have a significant impact on human physiology.
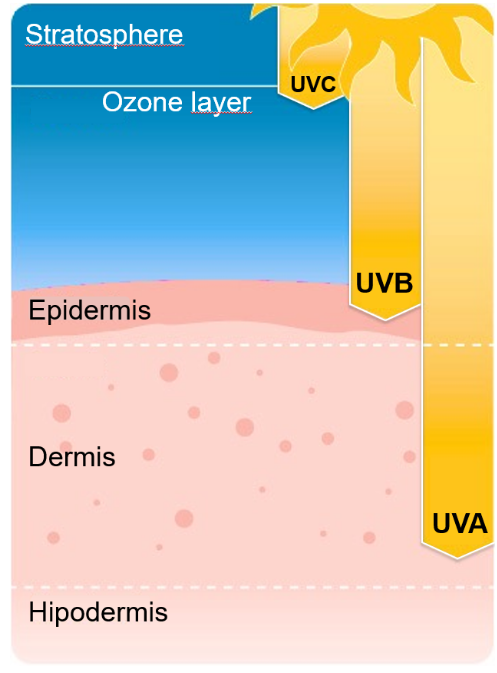
Figure 1. Forms of solar UV radiation and the degrees to which they reach our skin.
How UV Radiation Is Converted into Vitamin D
When we expose ourselves to sunlight, the UVB radiation is absorbed in the epidermis (the outer layer of our skin) by a molecule called 7-dehydrocholesterol causing it to be converted into previtamin D3. Previtamin D3 is easily transformed into vitamin D3, which exits the skin and diffuses into circulation, reaching the liver.
In the liver, it is converted by one or more enzymes into 25-hydroxyvitamin D3 [25(OH)D3].2, 4 It can then reach the kidneys, where it will be further metabolized into the “active” form of vitamin D: 1α,25-dihydroxyvitamin D3 [1α,25(OH)2D3].2, 4
Once formed, the D3 travels to the cells of virtually all tissues and organs in the body, where it will bind specific receptors. There is good evidence that various cells in other tissues besides the kidney can convert 25OHD3 into 1α,25(OH)2D3. This locally synthesized 1α,25(OH)2D3 can then bind the VDR in those cells or in nearby cells (figure 2).
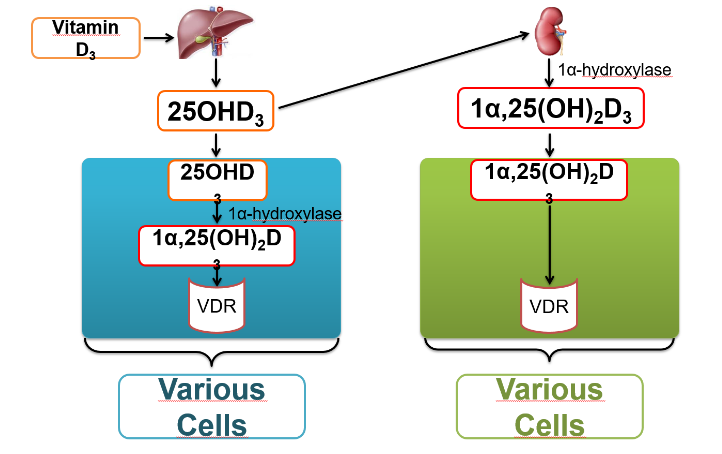
Figure 2. Formation of the active form of vitamin D3 and its influence on nearly 2000 genes within cells throughout the body.
The binding of 1α,25(OH)2D3 (either from the kidneys or derived from local production) to the VDR will affect the expression of approximately 2,000 genes and regulate many cellular processes.2, 4
This explains why vitamin D insufficiency is associated with all-cause mortality and many health problems, such as musculoskeletal disorders (e.g., rickets, osteomalacia, osteoporosis, muscle pain, sarcopenia), various types of cancer, hypertension, cardiovascular disease, infectious and autoimmune diseases (e.g., multiple sclerosis, inflammatory bowel disease, rheumatoid arthritis, systemic lupus erythematosus, diabetes, psoriasis), pregnancy complications, neurodegenerative diseases, depression, and even schizophrenia.4-8
Getting Enough Vitamin D
This fits with the evolutionary template, which states that some degree of sun exposure is necessary for optimal health. A sun-rich environment supposedly characterized the ecological niches of most of our hunter-gatherer ancestors32 until about 40 to 60 thousand years ago when a significant number of humans migrated to higher latitudes33 (although extreme latitudes appear to have only been systematically occupied more recently).34-36
Given the above evidence coupled with the results of a recent study that observed higher mortality rates among Swedish women who avoided sun exposure,30, 31 it can be assumed that sunlight regulates human physiology in many ways. It also suggests that replacing sun exposure with vitamin D3 (either through supplementation or diet) is a simplistic approach, but necessary when sunlight isn’t as available (such as in winter).
References
[1] Sklar LR, Almutawa F, Lim HW, Hamzavi I. Effects of ultraviolet radiation, visible light, and infrared radiation on erythema and pigmentation: a review. Photochem Photobiol Sci. 2013 Jan;12(1):54–64.
[2] Holick MF. Biological Effects of Sunlight, Ultraviolet Radiation, Visible Light, Infrared Radiation and Vitamin D for Health. Anticancer Res. 2016 Mar;36(3):1345–56.
[3] Diffey BL. What is light? Photodermatol Photoimmunol Photomed. 2002 Apr;18(2):68–74.
[4] Berridge MJ. Vitamin D cell signalling in health and disease. Biochem Biophys Res Commun. 2015 Apr 24;460(1):53-71.
[5] Wacker M, Holick MF. Sunlight and Vitamin D: A global perspective for health. dermatoendocrinology. 2013 Jan 1;5(1):51–108.
[6] Hewison M. Vitamin D and immune function: an overview. Proc Nutr Soc. 2012 Feb;71(1):50-61.
[7] Grant WB. Roles of Solar UVB and Vitamin D in Reducing Cancer Risk and Increasing Survival. Anticancer Res. 2016 Mar;36(3):1357-70.
[8] Pludowski P, Holick MF, Pilz S, et al. Vitamin D effects on musculoskeletal health, immunity, autoimmunity, cardiovascular disease, cancer, fertility, pregnancy, dementia and mortality-a review of recent evidence. Autoimmun Rev. 2013 Aug;12(10):976-89.
[9] Bäärnhielm M, Hedström AK, Kockum I, et al. Sunlight is associated with decreased multiple sclerosis risk: no interaction with human leukocyte antigen-DRB1*15. Eur J Neurol. 2012 Jul;19(7):955-62.
[10] Becklund BR, Severson KS, Vang SV, DeLuca HF. UV radiation suppresses experimental autoimmune encephalomyelitis independent of vitamin D production. Proc Natl Acad Sci USA. 2010 Apr 6;107(14):6418–23.
[11] Hart PH, Gorman S, Finlay-Jones JJ. Modulation of the immune system by UV radiation: more than just the effects of vitamin D? Nat Rev Immunol. 2011 Aug 19;11(9):584-96.
[12] Hart PH, Gorman S. Exposure to UV Wavelengths in Sunlight Suppresses Immunity. To What Extent is UV-induced Vitamin D3 the Mediator Responsible? Clin Biochem Rev. 2013 Feb;34(1):3-13.
[13] Juzeniene A, Moan J. Beneficial effects of UV radiation other than via vitamin D production. dermatoendocrinology. 2012 Apr 1;4(2):109–17.
[14] Jussila A, Huotari-Orava R, Ylianttila L, Partonen T, Snellman E. Narrow-band ultraviolet B radiation induces the expression of β-endorphin in human skin in vivo. J Photochem Photobiol B. 2016 Feb;155:104-8.
[15] Skobowiat C, Dowdy JC, Sayre RM, Tuckey RC, Slominski A. Cutaneous hypothalamic-pituitary-adrenal axis homolog: regulation by ultraviolet radiation. Am J Physiol Endocrinol Metab. 2011 Sep;301(3):E484-93.
[16] Wintzen M, Yaar M, Burbach JP, Gilchrest BA. Proopiomelanocortin gene product regulation in keratinocytes. J Invest Dermatol. 1996 Apr;106(4):673-8.
[17] Fell GL, Robinson KC, Mao J, Woolf CJ, Fisher DE. Skin β-endorphin mediates addiction to UV light. Cell. 2014 Jun 19;157(7):1527-34.
[18] Walch JM, Rabin BS, Day R, Williams JN, Choi K, Kang JD. The effect of sunlight on postoperative analgesic medication use: a prospective study of patients undergoing spinal surgery. Psychosom Med. 2005 Jan-Feb;67(1):156-63.
[19] Zanello SB, Jackson DM, Holick MF. Expression of the circadian clock genes clock and period1 in human skin. J Invest Dermatol. 2000 Oct;115(4):757-60.
[20] Matsui MS, Pelle E, Dong K, Pernodet N. Biological Rhythms in the Skin. Int J Mol Sci. 2016 May 24;17(6).
[21] Kawara S, Mydlarski R, Mamelak AJ, et al. Low-dose ultraviolet B rays alter the mRNA expression of the circadian clock genes in cultured human keratinocytes. J Invest Dermatol. 2002 Dec;119(6):1220-3.
[22] Jurvelin H, Jokelainen J, Takala T. Transcranial bright light and symptoms of jet lag: a randomized, placebo-controlled trial. Aerosp Med Hum Perform. 2015 Apr;86(4):344-50.
[23] Weyland PG, Grant WB, Howie-Esquivel J. Does sufficient evidence exist to support a causal association between vitamin D status and cardiovascular disease risk? An assessment using Hill’s criteria for causality. Nutrients. 2014 Sep 2;6(9):3403-30.
[24] Grimes DS, Hindle E, Dyer T. Sunlight, cholesterol and coronary heart disease. QJM. 1996 Aug;89(8):579-89.
[25] DuBroff R, de Lorgeril M. Cholesterol confusion and statin controversy. World J Cardiol. 2015 Jul 26;7(7):404-9.
[26] Johnson RS, Titze J, Weller R. Cutaneous control of blood pressure. Curr Opin Nephrol Hypertens. 2016 Jan;25(1):11-5.
[27] Opländer C, Volkmar CM, Paunel-Görgülü A, et al. Whole body UVA irradiation lowers systemic blood pressure by release of nitric oxide from intracutaneous photolabile nitric oxide derivates. Circ Res. 2009 Nov 6;105(10):1031-40.
[28] Liu D, Fernandez BO, Hamilton A, et al. UVA irradiation of human skin vasodilates arterial vasculature and lowers blood pressure independently of nitric oxide synthase. J Invest Dermatol. 2014 Jul;134(7):1839-46.
[29] Feelisch M, Kolb-Bachofen V, Liu D, Lundberg JO, Revelo LP, Suschek CV, Weller RB. Is sunlight good for our heart? Eur Heart J. 2010 May;31(9):1041-5.
[30] Lindqvist PG, Epstein E, Landin-Olsson M, et al. Avoidance of sun exposure is a risk factor for all-cause mortality: results from the Melanoma in Southern Sweden cohort. J Intern Med. 2014 Jul;276(1):77-86.
[31] Lindqvist PG, Epstein E, Nielsen K, Landin-Olsson M, Ingvar C, Olsson H. Avoidance of sun exposure as a risk factor for major causes of death: a competing risk analysis of the Melanoma in Southern Sweden cohort. J Intern Med. 2016 Oct;280(4):375-87.
[32] Jablonski NG, Chaplin G. Colloquium paper: human skin pigmentation as an adaptation to UV radiation. Proc Natl Acad Sci U S A. 2010 May 11;107 Suppl 2:8962-8.
[33] López S, van Dorp L, Hellenthal G. Human Dispersal Out of Africa: A Lasting Debate. Evol Bioinform Online. 2016 Apr 21;11(Suppl 2):57-68.
[34] Liu H, Prugnolle F, Manica A, Balloux F. A geographically explicit genetic model of worldwide human-settlement history. Am J Hum Genet. 2006 Aug;79(2):230-7.
[35] Chaplin G, Jablonski NG. The human environment and the vitamin D compromise: Scotland as a case study in human biocultural adaptation and disease susceptibility. Hum Biol. 2013 Aug;85(4):529-52.
[36] Oppenheimer S. Out-of-Africa, the peopling of continents and islands: tracing uniparental gene trees across the map. Philos Trans R Soc Lond B Biol Sci. 2012 Mar 19;367(1590):770-84.
The Paleo Diet Team
The Paleo Diet® team consists of a group of scientists, journalists, experts, and recipe creators who stay at the forefront of nutrition science.
More About The Author



