Why The Paleo Diet Supports a Low Sodium Diet

Salt, and its addition to many of the foods we eat, has steadily become one of the more controversial topics in the nutrition world. How much is too much? How much, if any, do we need? Is salt Paleo?
In an effort to reduce the average American’s high salt intake, the FDA recently asked food companies to voluntarily reduce the sodium content of their products.
Since a large portion of added sodium in the average American diet comes from processed food, the idea is that this shift will help bring the average American diet down to the recommended daily allowance (RDA) of 2,300mg of salt per day. [1] The typical American consumes much more than this at about 3,400mg of sodium per day.
We applaud the FDA for trying to help Americans cut back on sodium, as a low-salt diet is a key part of The Paleo Diet®.
We also recognize that this is a tough challenge. Humans crave salt and will favor foods that are high in sodium. Let’s dive into why that is.
Why Do We Crave Salt and Sugar?
There are two foods that humans crave above all else—sugar and salt. The food science industry understands this well and works hard to develop foods that tickle every nerve when it comes to these cravings. This is why you’ll see sugar and salt as primary ingredients on most processed food products.
While there has been some debate about sodium, everyone agrees about the dangers of sugar—particularly processed sugar. It is one of the main drivers of our current epidemic of obesity, metabolic disease, and diabetes [2–4].
It is a less accepted notion that salt carries such dramatic health risks—particularly within the broader Paleo space. However, research finds that salt contributes to chronic diseases, including cardiovascular disease, autoimmune disease, and certain cancers. [5–16]
So, why do we crave salt and sugar? There’s an evolutionary explanation for it. The truth is that we do need at least small amounts of salt and some simple sugars to survive. Our bodies need sodium for almost all physiological functions, and despite some ketogenic diet misconceptions, our brains need glucose to function.
In Paleolithic times, both salt and simple sugars were rare. So, our bodies developed to make sure that when we encountered them, we ate them. That was the magic formula—necessary but rare—for the evolution of strong cravings. Overconsumption was never an issue, so even though our ancestors craved it, they necessarily kept their intake low. That is, until modern times.
Why Do Some Say a High-Sodium Diet Is Healthy?
Most influencers in Paleolithic eating were quick to recognize the dangers of consuming too much sugar. In fact, some have shifted to a ketogenic lifestyle, which virtually eliminates simple sugar from the diet. Yet, when it comes to salt, many of these same influencers have taken a very different direction.
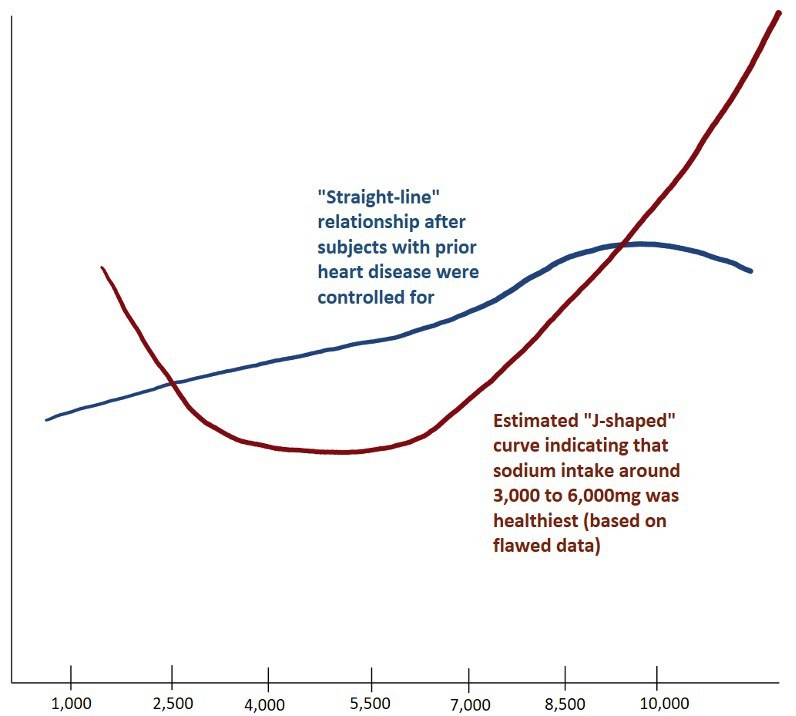
In fact, there has been a trend towards promoting a diet even higher in salt! [17] This trend grew out of some highly publicized research, specifically two studies published in 2014. These studies showed that while people on a very high-sodium diet had much higher rates of heart disease, likewise, so did people on a very low sodium diet. [18–20]
It created a U- or J-shaped relationship, with the healthiest people at the bottom of the “J” curve eating around 3,000 to 6,000mg of sodium per day—which, even on the low end, is well above the recommendation of 2,300mg of sodium per day. This has led some to believe that eating even twice the RDA of sodium would improve their health.
The problem is that these studies had two fundamental flaws that caused them to mis-represent the data.
Some High-Salt Diet Research Is Flawed
Before you walk away thinking that 3,000-6,000mg of salt per day is the way to go, let’s take a closer look at the flaws in these studies.
First, these studies did not use the “gold standard” 24-hour urinary sodium measurement, the importance of which Dr. Cordain explains in detail in this article.
Second, and more critical to understand, is that the researchers did not control for people who already had heart disease at the start of the study. That’s important because when someone is diagnosed with heart disease, one of the first things doctors generally recommend is a reduction in sodium intake. So, it wasn’t that a very low sodium diet was causing high rates of heart disease. It was heart disease that was causing a very low sodium diet!
A research team identified this second flaw, and in 2016 they analyzed data from a larger study tracking 3,126 subjects over 20 years. This time, the researchers controlled for subjects who had been diagnosed with heart disease prior to the study. When they did that, the J-shaped relationship disappeared and it became a straight line—the lower the sodium in the subjects’ diets, the lower the risk of heart disease. In fact, the risk of all causes of death were lower.
On Sodium, The Paleo Diet Agrees with the Food & Drug Administration
We recently received an email from a reader criticizing our position because we were in alignment with the RDAs of several micronutrients. There was an implication that if we agreed with the FDA or USDA on anything, we’d lose credibility.
Our position is always the same—we follow the science. When our assessment of the science matches the messaging of the FDA, we’re all the happier. We see no reason to disagree with the FDA or the USDA for its own sake. In this case, we fully support the FDA’s push to encourage processed food companies to reduce their high sodium levels.
We have always promoted a low-sodium diet here at The Paleo Diet and in this case, we believe the current RDA of 2,300mg per day is at the high end of what we should consume.
Five Reasons The Paleo Diet Is a Low Sodium Diet
We have written extensively about sodium and its health implications over the past few years. Since there is so much information to comb through, here are five of our key takeaways to help you understand why we stand behind a low-sodium diet.
1. It’s nearly impossible to eat too much sodium on The Paleo Diet.
The good news is that if you’re eating a true Paleo Diet and staying away from added salt, you simply won’t hit the upper levels of sodium. Dr. Cordain wrote extensively about this in a response to a reader who defended the idea that 3,000 to 7,000mg of sodium per day is healthy. Even if you’re eating 2,500 calories per day of only Paleo foods, it is virtually impossible to eat more than the RDA of sodium.
If we look to the typical hunter-gatherer society, we can see that they ate very little sodium—less than 1,200mg per day. [13] A typical modern Paleo Diet with no added salt usually falls in the 1,600-2,200mg range and even lower if you eat more fruits than vegetables.
2. Too much sodium increases inflammation, which can lead to many chronic diseases.
The science behind how excess salt contributes to inflammation is very complex, and covered in more detail in two articles by Marc Bubbs and Dr. Loren Cordain. As a quick explanation, salt collects in our cells, which causes an increase in two highly inflammatory immune cells called CD14+ macrophages and Th17 cells. [10,15] Imbalances in these two cell types have been connected with almost all autoimmune diseases, heart disease, and some cancers. [15,21–27]
3. Excess sodium contributes to cardiovascular disease.
As I mentioned earlier, there is a straight-line relationship between sodium consumption and heart disease. In other words, the more you consume, the higher your risk. [20] This is due in part to the inflammation mentioned above. Plus, as Dr. Cordain detailed in a recent article, too much sodium can contribute to key steps in the formation of the atherosclerotic plaque in our arteries that in turn lead to heart attack and stroke. [28–34]
4. Too much sodium can contribute to cancer.
An increased risk of cancer is another consequence of the accumulation of excess sodium within our cells. It does so by damaging our DNA, increasing oxidative stress, and fundamentally impairing metabolism within the cells—an effect called the Warburg metabolism. [35-42] Increasing the ratio of potassium to sodium in our diets can prevent many of the negative effects. That brings us to our fifth and most important point.
5. Increasing potassium while reducing sodium can reverse many of these negative health effects.
Sodium and potassium have a synergistic relationship. The ideal ratio in our bodies is between 5 to 1 and 10 to 1 potassium to sodium. But the typical Western diet flips the ratio and can have twice the sodium as potassium or worse. [43] As Dr. Mark J. Smith explained in this article, all of our cells use potassium to pump sodium out of cells, which helps reverse many of the inflammatory effects detailed above. When the sodium-to-potassium ratio in our diet resets to its natural level, research shows that it has a protective effect against cancer, reduces blood pressure, and even prevent bone loss [19,44–51]. Our best sources of potassium are vegetables and fruit, and it is nearly impossible to eat enough of these healthy foods on a high sodium diet to reach a healthy ratio of 5-to-1 or better.
[1] Curley C. Pass the Salt: FDA Issues New Guidelines on Sodium in Foods. Healthline 2021. https://www.healthline.com/hea… (accessed November 8, 2021).
[2] Kearns CE, Schmidt LA, Glantz SA. Sugar Industry and Coronary Heart Disease Research: A Historical Analysis of Internal Industry Documents. Jama Intern Med 2016;176:1680. https://doi.org/10.1001/jamain…;
[3] Pase MP, Himali JJ, Beiser AS, Aparicio HJ, Satizabal CL, Vasan RS, et al. Sugar- and Artificially Sweetened Beverages and the Risks of Incident Stroke and Dementia. Stroke 2017;48:1139–46. https://doi.org/10.1161/stroke…;
[4] Pase MP, Himali JJ, Jacques PF, DeCarli C, Satizabal CL, Aparicio H, et al. Sugary beverage intake and preclinical Alzheimer’s disease in the community. Alzheimer’s Dementia 2017;13:955–64. https://doi.org/10.1016/j.jalz…;
[5] He FJ, MacGregor GA. A comprehensive review on salt and health and current experience of worldwide salt reduction programmes. J Hum Hypertens 2009;23:363–84. https://doi.org/10.1038/jhh.20…;
[6] Meer JWM van der, Netea MG. A Salty Taste to Autoimmunity. New Engl J Medicine 2013;368:2520–1. https://doi.org/10.1056/nejmci…;
[7] Ge S, Feng X, Shen L, Wei Z, Zhu Q, Sun J. Association between Habitual Dietary Salt Intake and Risk of Gastric Cancer: A Systematic Review of Observational Studies. Gastroent Res Pract 2012;2012:808120. https://doi.org/10.1155/2012/8…;
[8] Yi B, Titze J, Rykova M, Feuerecker M, Vassilieva G, Nichiporuk I, et al. Effects of dietary salt levels on monocytic cells and immune responses in healthy human subjects: a longitudinal study. Transl Res 2015;166:103–10. https://doi.org/10.1016/j.trsl…;
[9] D’Elia L, Rossi G, Ippolito R, Cappuccio FP, Strazzullo P. Habitual salt intake and risk of gastric cancer: A meta-analysis of prospective studies. Clin Nutr 2012;31:489–98. https://doi.org/10.1016/j.clnu…;
[10] Wu C, Yosef N, Thalhamer T, Zhu C, Xiao S, Kishi Y, et al. Induction of pathogenic Th17 cells by inducible salt sensing kinase SGK1. Nature 2013;496:513–7. https://doi.org/10.1038/nature…;
[11] Cook NR, Appel LJ, Whelton PK. Lower Levels of Sodium Intake and Reduced Cardiovascular Risk. Circulation 2014;129:981–9. https://doi.org/10.1161/circul…;
[12] O’Shea JJ, Jones RG. Rubbing salt in the wound. Nature 2013;496:437–9. https://doi.org/10.1038/nature…;
[13] Denton D. Salt intake and high blood pressure in man. Primitive peoples, unacculturated societies: with comparisons. The Hunger for Salt, An Anthropological, Physiological and Medical Analysis, New York: Springer-Verlag; 1984, p. 556–84.
[14] Hu J, Vecchia CL, Morrison H, Negri E, Mery L, Group CCRER. Salt, processed meat and the risk of cancer. Eur J Cancer Prev 2011;20:132–9. https://doi.org/10.1097/cej.0b…;
[15] Kleinewietfeld M, Manzel A, Titze J, Kvakan H, Yosef N, Linker RA, et al. Sodium chloride drives autoimmune disease by the induction of pathogenic TH17 cells. Nature 2013;496:518–22. https://doi.org/10.1038/nature…;
[16] Zhou X, Zhang L, Ji W-J, Yuan F, Guo Z-Z, Pang B, et al. Variation in Dietary Salt Intake Induces Coordinated Dynamics of Monocyte Subsets and Monocyte-Platelet Aggregates in Humans: Implications in End Organ Inflammation. Plos One 2013;8:e60332. https://doi.org/10.1371/journa…;
[17] Kresser C. Shaking Up The Salt Myth: Healthy Salt Recommendations 2012. http://chriskresser.com/shaking-up-the-salt-myth-healthy-salt- recommendations/.
[18] Pfister R, Michels G, Sharp SJ, Luben R, Wareham NJ, Khaw K. Estimated urinary sodium excretion and risk of heart failure in men and women in the EPIC‐Norfolk study. Eur J Heart Fail 2014;16:394–402. https://doi.org/10.1002/ejhf.5…;
[19] O’Donnell M, Mente A, Rangarajan S, McQueen MJ, Wang X, Liu L, et al. Urinary Sodium and Potassium Excretion, Mortality, and Cardiovascular Events. New Engl J Medicine 2014;371:612–23. https://doi.org/10.1056/nejmoa…;
[20] Cook NR, Appel LJ, Whelton PK. Sodium Intake and All-Cause Mortality Over 20 Years in the Trials of Hypertension Prevention. J Am Coll Cardiol 2016;68:1609–17. https://doi.org/10.1016/j.jacc…;
[21] Faraco G, Brea D, Garcia-Bonilla L, Wang G, Racchumi G, Chang H, et al. Dietary salt promotes neurovascular and cognitive dysfunction through a gut-initiated TH17 response. Nat Neurosci 2018;21:240–9. https://doi.org/10.1038/s41593…;
[22] Haase S, Haghikia A, Wilck N, Müller DN, Linker RA. Impacts of microbiome metabolites on immune regulation and autoimmunity. Immunology 2018;154:230–8. https://doi.org/10.1111/imm.12…;
[23] Wilck N, Matus MG, Kearney SM, Olesen SW, Forslund K, Bartolomaeus H, et al. Salt-responsive gut commensal modulates TH17 axis and disease. Nature 2017;551:585–9. https://doi.org/10.1038/nature…;
[24] LI Q, LI Q, CHEN J, LIU Y, ZHAO X, TAN B, et al. Prevalence of Th17 and Treg cells in gastric cancer patients and its correlation with clinical parameters. Oncol Rep 2013;30:1215–22. https://doi.org/10.3892/or.201…;
[25] Chang SH. T helper 17 (Th17) cells and interleukin-17 (IL-17) in cancer. Arch Pharm Res 2019;42:549–59. https://doi.org/10.1007/s12272…;
[26] Ding H-S, Yang J, Yang J, Ding J-W, Chen P, Zhu P. Interleukin-17 contributes to cardiovascular diseases. Mol Biol Rep 2012;39:7473–8. https://doi.org/10.1007/s11033…;
[27] Du Y-N, Tang X-F, Xu L, Gao PJ, Han WQ. Th17/Treg Imbalance in Hypertension. Cardiovasc Pharmacol Open Access 2018;7:1–3. https://doi.org/10.4172/2329-6…;
[28] Dmitrieva NI, Burg MB. Elevated Sodium and Dehydration Stimulate Inflammatory Signaling in Endothelial Cells and Promote Atherosclerosis. Plos One 2015;10:e0128870. https://doi.org/10.1371/journa…;
[29] Wild J, Soehnlein O, Dietel B, Urschel K, Garlichs CD, Cicha I. Rubbing salt into wounded endothelium: Sodium potentiates proatherogenic effects of TNF-? under non-uniform shear stress. Thromb Haemostasis 2014;112:183–95. https://doi.org/10.1160/th13-1…;
[30] Dickinson KM, Clifton PM, Burrell LM, Barrett PHR, Keogh JB. Postprandial effects of a high salt meal on serum sodium, arterial stiffness, markers of nitric oxide production and markers of endothelial function. Atherosclerosis 2014;232:211–6. https://doi.org/10.1016/j.athe…;
[31] Edwards DG, Farquhar WB. Vascular effects of dietary salt. Curr Opin Nephrol Hy 2015;24:8–13. https://doi.org/10.1097/mnh.00…;
[32] Kusche-Vihrog K, Schmitz B, Brand E. Salt controls endothelial and vascular phenotype. Pflügers Archiv – European J Physiology 2015;467:499–512. https://doi.org/10.1007/s00424…;
[33] Oberleithner H, Riethmüller C, Schillers H, MacGregor GA, Wardener HE de, Hausberg M. Plasma sodium stiffens vascular endothelium and reduces nitric oxide release. Proc National Acad Sci 2007;104:16281–6. https://doi.org/10.1073/pnas.0…;
[34] Jeggle P, Hofschröer V, Maase M, Bertog M, Kusche‐Vihrog K. Aldosterone synthase knockout mouse as a model for sodium‐induced endothelial sodium channel up‐regulation in vascular endothelium. Faseb J 2016;30:45–53. https://doi.org/10.1096/fj.14-…;
[35] Dmitrieva NI, Cai Q, Burg MB. Cells adapted to high NaCl have many DNA breaks and impaired DNA repair both in cell culture and in vivo. P Natl Acad Sci Usa 2004;101:2317–22. https://doi.org/10.1073/pnas.0…;
[36] Burg MB, Ferraris JD, Dmitrieva NI. Cellular Response to Hyperosmotic Stresses. Physiol Rev 2007;87:1441–74. https://doi.org/10.1152/physre…;
[37] Dmitrieva NI, Burg MB. Analysis of DNA breaks, DNA damage response, and apoptosis produced by high NaCl. Am J Physiol-Renal 2008;295:F1678–88. https://doi.org/10.1152/ajpren…;
[38] Jin K, Vaziri ND. Salt-sensitive hypertension in mitochondrial superoxide dismutase deficiency is associated with intra-renal oxidative stress and inflammation. Clin Exp Nephrol 2014;18:445–52. https://doi.org/10.1007/s10157…;
[39] Dornas WC, Lima WG de, Santos RC dos, Guerra JF da C, Souza MO de, Silva M, et al. High dietary salt decreases antioxidant defenses in the liver of fructose-fed insulin-resistant rats. J Nutritional Biochem 2013;24:2016–22. https://doi.org/10.1016/j.jnut…;
[40] Zhou X, Ferraris JD, Cai Q, Agarwal A, Burg MB. Increased reactive oxygen species contribute to high NaCl-induced activation of the osmoregulatory transcription factor TonEBP/OREBP. Am J Physiol-Renal 2005;289:F377–85. https://doi.org/10.1152/ajpren…;
[41] Warburg O, Wind F, Negelein E. THE METABOLISM OF TUMORS IN THE BODY. J Gen Physiology 1927;8:519–30. https://doi.org/10.1085/jgp.8….;
[42] Amara S, Zheng M, Tiriveedhi V. Oleanolic Acid Inhibits High Salt-Induced Exaggeration of Warburg-like Metabolism in Breast Cancer Cells. Cell Biochem Biophys 2016;74:427–34. https://doi.org/10.1007/s12013…;
[43] Bailey RL, Parker EA, Rhodes DG, Goldman JD, Clemens JC, Moshfegh AJ, et al. Estimating Sodium and Potassium Intakes and Their Ratio in the American Diet: Data from the 2011–2012 NHANES. J Nutrition 2015;146:745–50. https://doi.org/10.3945/jn.115…;
[44] L. F, C. M R, E. S D, K. T, A. S. Diet, evolution and aging – The pathophysiologic effects of the post-agricultural inversion of the potassium-to-sodium and base-to-chloride ratios in the human diet. European Journal of Nutrition 2001;40:200–13. https://doi.org/10.1007/s394-0…;
[45] Jansson B. Geographic cancer risk and intracellular potassium/sodium ratios. Cancer Detect Prev 1986;9:171–94.
[46] Cook NR, Obarzanek E, Cutler JA, Buring JE, Rexrode KM, Kumanyika SK, et al. Joint Effects of Sodium and Potassium Intake on Subsequent Cardiovascular Disease: The Trials of Hypertension Prevention Follow-up Study. Arch Intern Med 2009;169:32–40. https://doi.org/10.1001/archin…;
[47] Potassium Citrate Prevents Increased Urine Calcium Excretion and Bone Resorption Induced by a High Sodium Chloride Diet.pdf n.d.
[48] Jansson B. Potassium, sodium, and cancer: a review. J Environ Pathology Toxicol Oncol Official Organ Int Soc Environ Toxicol Cancer 1996;15:65–73.
[49] Manger WM, Simchon S, Stier CT, Loscalzo J, Jan K-M, Jan R, et al. Protective effects of dietary potassium chloride on hemodynamics of Dahl salt-sensitive rats in response to chronic administration of sodium chloride. J Hypertens 2003;21:2305–13. https://doi.org/10.1097/000048…;
[50] Aaron KJ, Sanders PW. Role of Dietary Salt and Potassium Intake in Cardiovascular Health and Disease: A Review of the Evidence. Mayo Clin Proc 2013;88:987–95. https://doi.org/10.1016/j.mayo…;
[51] Perez V, Chang ET. Sodium-to-Potassium Ratio and Blood Pressure, Hypertension, and Related Factors. Adv Nutrition Int Rev J 2014;5:712–41. https://doi.org/10.3945/an.114…;
Trevor Connor, M.S.
Dr. Loren Cordain’s final graduate student, Trevor Connor, M.S., brings more than a decade of nutrition and physiology expertise to spearhead the new Paleo Diet team.
More About The Author




